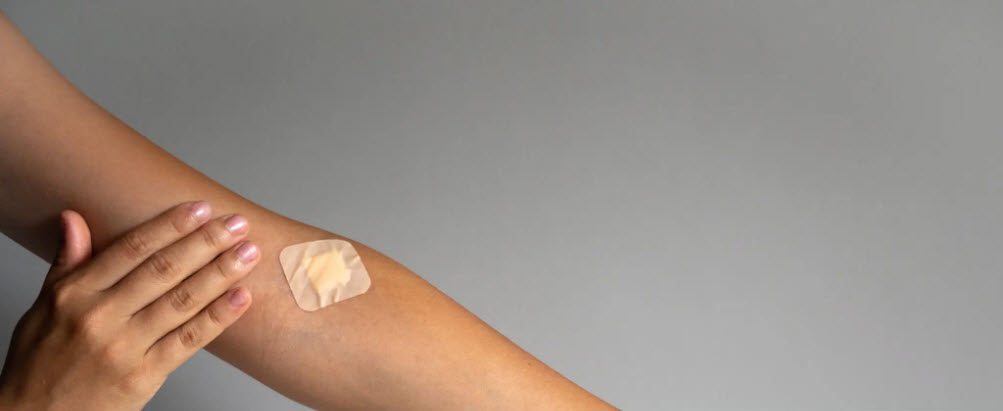
Cannabis patches work. Maybe that’s a problem.
For years, Jennifer Mansour felt them coming.
“You can’t stop one,” she said. “As soon as I’d notice that the lights felt a little too bright, I knew I was done for. I’d tell my boss, and then I’d get in the car and pop on my sunglasses because I could feel another one coming on, and I couldn’t do a thing to stop it.”
There’s no cure for migraines, and sufferers usually find their own ways to cope—strong headache medicine, blackout curtains, meditation. Overusing NSAIDs, the only thing that really helps, creates its own problems. Mansour needed a different painkiller. Then she heard about transdermal cannabis patches.
“Migraines can come on due to what you eat and drink, like alcohol or coffee, so you get used to basically ‘saying no to drugs’ when you’re little,” she said. She discovered the patch on TikTok, where, she says, she converted. For Mansour, the patches function as advertised, dulling her pain and relaxing her muscles. “I stick one on the top of my foot, and in about 20 minutes, it hits me,” she said. “It relaxes my shoulders and neck. That’s where I store tension.”
But for every Mansour, there’s a James Mesh. A 38-year-old drywaller, he deals with back pain the way most of us deal with email. Most mornings, he washes down four ibuprofen with a Monster energy drink. He tried transdermal patches, too. Didn’t work.
 “I searched it up, called the shop, and went down and bought a big roll. I ended up giving most away. I don’t know if I sweated too much or what for them to work, but I never felt a thing,” he said. “It was really just like going to work any old day.”
“I searched it up, called the shop, and went down and bought a big roll. I ended up giving most away. I don’t know if I sweated too much or what for them to work, but I never felt a thing,” he said. “It was really just like going to work any old day.”
An Inconvenient Truth
Transdermal patches have become a staple in modern medicine, treating conditions as varied as heart problems and Parkinson’s disease. The steady dosage they deliver makes them ideal couriers for a wide variety of drugs, from lidocaine to nicotine to estrogen. But cannabis presents a tough case.
Unlike those other compounds, THC and CBD exhibit hydrophobic properties, so they’re not especially good at passing through human skin. Because our skin is mostly water, and each person’s dermal layers are unique, the effectiveness of transdermals can vary from person to person. Just because CBD relieves Mansour’s headaches doesn’t mean Mesh was lying when he spent the day with an achy back.
This might be because Mesh has, literally, thicker skin, or maybe he didn’t take enough. It’s hard to gauge how much cannabis a patch delivers. A 40 mg transdermal that lasts for 10 hours will, at best, deliver 2mg of active ingredients per hour. For experienced users, that may be too low to register. It’s also possible that patch placement affects the process. The common advice of applying transdermal to veinous regions, like the inner wrist, rests on the theory that the active ingredients will have an easier time passing through thin skin.
As tidy as these explanations are, they’re not what keeps transdermals from gaining popularity. People don’t clamor for a patch because they can’t get you high. Not really. Although patches allow THC and CBD to pass into the bloodstream, it never gets metabolized by the liver. Scientifically, patches cannot produce psychoactive effects. That makes them the best example of cannabis medicine that has been produced so far. But by existing as all relief, no buzz, they betray a certain truth about cannabis users. One that, as it turns out, is the central issue surrounding transdermal patches.
For years, a sizable portion of cannabis enthusiasts have sworn by its medicinal potential. Advocates pushed for legality, citing its potential to transform treatments for pain, seizures, and cancer. The fact that it got people high was beside the point. Like a majority of functional medicines, they argued, cannabis use comes with side effects. But, as patches prove, once that side effect is nullified, the cannabis option becomes less appealing for potential users. Or at least some of them.
 Internet communities dedicated to dealing with issues such as arthritis, migraines, cancer, and chronic pain are united in their efforts to prove to naysayers that patches don’t interfere with cognitive function. Many of these groups openly advocate for the right to use patches at work, yet no state legislature will take up the cause. Why not? Bias—this time from the other side. The anti-cannabis crowd should be thrilled someone subtracted fun from the equation. Yet many skeptics still look sideways at cannabis-based treatments.
Internet communities dedicated to dealing with issues such as arthritis, migraines, cancer, and chronic pain are united in their efforts to prove to naysayers that patches don’t interfere with cognitive function. Many of these groups openly advocate for the right to use patches at work, yet no state legislature will take up the cause. Why not? Bias—this time from the other side. The anti-cannabis crowd should be thrilled someone subtracted fun from the equation. Yet many skeptics still look sideways at cannabis-based treatments.
When pressed, every subject interviewed for this article admitted to following a don’t-ask, don’t-tell policy at the office: They simply slap on a patch without alerting their bosses. A few pointed to the recent wins in public schools as a reason for optimism. In 2018, the family of an Illinois teenager with Leukemia successfully lobbied the state to allow patch use during school for students with medical marijuana prescriptions. Since the passage of “Ashley’s Law,” five more states have used it as a guide for incorporating doctor-prescribed cannabis in public schools.
Despite the momentum, few expressed hope for real change. “With A.I. coming, they look for any reason to fire you,” said one patch user who asked to remain anonymous. “If you fail a blood test, it doesn’t matter if you never got high. That’s just another reason for them to let you go.”
Unemployment would have one upside, the patch user added. “If I got fired? Well, I guess I could finally get high.”